If you think about technology as simply being able to do more with less, healthcare is a great place to apply those skills” Steve Krupa, CEO, Psilos Group
On March 11th, 2020, the World Health Organization officially declared the COVID-19 outbreak a global pandemic. 3 years later there seems to be a shared feeling of disappointment about how little healthcare systems have changed despite often proving to be inadequate when put under the significant stress of COVID-19. While structural and technological progress has indeed been slower than expected, there is no doubt the healthcare sector is experiencing a technology-driven evolution that slowly but inexorably, will change the way we handle our health. Between 2018 and 2022 the healthcare sector has attracted $415 billion dollars in venture capital investment, the highest volume among all sectors globally1, signaling confidence from the market that there is still plenty of room for innovation and growth in global healthcare. The market’s confidence in the innovations of this historically traditional industry is evident through several positive indicators, such as governments lowering legislative barriers and increasingly opening up to collaborations with the private sector. Overall, we can positively say that a new mindset has been established: healthtech is no longer seen as a nice-to-have “add-on” to healthcare. It is a key ally in the effort to make healthcare more accessible, agile and effective. At the same time, health-tech implementation is a prerequisite to successfully competing as a business operator in the future.
Successful innovators start with current issues to envision what a better future could look like. We will try a similar approach and move through 6 challenges present across the healthcare value chain. Starting with today’s challenges, we will demonstrate how healthtech can improve the way: (1) lifestyles and prevention become an active tool to move from sickcare to healthcare, (2) patient medical records are made available, (3) new drugs are developed, (4) waiting lists and clinicians’ shortages are reduced, (5) patients adhere to prescribed treatments.
Unhealthy lifestyles
While a portion of pathologies are determined by a person’s genetic makeup, many others are linked to a person’s lifestyle. If we look at the United States, it is estimated that one in three Americans is likely to die prematurely from a condition closely related to lifestyle2, such as poor diet, smoking, lack of physical activity, excessive alcohol consumption. The focus on lifestyle improvement to prevent pathologies is not new. We can find academic research recommending that major health policies should emphasize reducing unhealthy lifestyles dating three decades ago3. While the importance of lifestyle improvement is clear, we’ve so far been ineffective at supporting people on their path to behavior change. Behavior modification requires continuous monitoring and follow-up, a level of care that is often unsustainable for traditional healthcare systems. Becoming more effective in supporting the population on their path to a healthier lifestyle is fundamental to minimize preventable pathologies. This is crucial in a context of severe scarcity of healthcare resources and steeply rising demand for care.
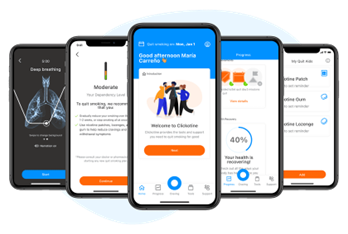
Digital Therapeutics (DTx) have proven to be an effective support for people as they learn and adapt to a new lifestyle. Digital therapeutics is a fairly new term referring to a group of digital products – apps or software – that can be used as self-standing therapy or in support of pharmacological therapy. Digital therapeutics have been the fastest growing area within the healthtech space in recent years, with global VC funding increasing 4x between 2017 and 20224. As attention from investors rises, so does consideration from regulators. While globlal regulatory agencies are still adapting to the fast growth of the digital therapy space, the American Food and Drug Administration (FDA) has already considered DTx as valid healing interventions for several years. Several DTx products focusing on behavior modification have received FDA clearance for prescription use. One example is Click Therapeutics’ Clickotine, a smartphone app aimed at helping users to quit smoking. Clickotine provides its users with a personalized treatment plan tailored to the user’s smoking habits, history and desired quit plan. The app, which utilizes principles of cognitive-behavioral therapy (CBT), empowers users to monitor their progress over time, providing motivation and craving management tools including guided breathing exercises, distraction techniques, and mindfulness practices. It is important to note that DTx effectiveness is not limited to lifestyle improvements: FDA approval has also been granted for DTx products that tackle chronic insomnia, attention deficit hyperactivity disorder (ADHD), panic and post-traumatic stress disorder, and drug addiction.
Prevention
Perhaps the largest impact digital technologies will have on healthcare will be to shift the focus from therapy to the care of people. Today, the center of care is the hospital, and the focus is on the treatment of acute cases. Our approach to illness is a reactive one as we wait for people to show symptoms before treating them: rather than providing healthcare, what we provide today is sickcare. The “patient journey” begins when a patient enters a healthcare facility, often through the emergency room, and it ends once the patient leaves the facility, with very little thought invested in what happened before or what will come after. As the tools at our disposal change and the proportion of the population affected by chronic conditions exponentially increases, it is time for our approach to care to evolve into a preventative model. If we manage to rely on digital tools and increase resolution at the primary care level, we will also decrease the number of acute cases, decrease healthcare spending and improve medical outcomes, all this while safeguarding hospital bed capacity. Three technologies that will primarily support us in this evolution are wearable monitoring devices, genomics, and artificial intelligence (AI).
Wearable monitoring devices allow for less invasive and continuous diagnostic analyses. They are particularly effective at preventing emergency situations by signaling potential conditions before the appearance of symptoms. By providing practitioners with a continuous flow of data that can be used for clinical decision making, wearable health monitoring devices reduce the need for patients to go to the hospital for routine visits, thus reducing the costs of care while also improving medical outcomes. The development of portable MinION devices by Oxford Nanopore in 2018 started the revolutionary age of personal genomics. Before MinION technology it was only possible to sequence strands of the human genome at a high cost in well-equipped labs. Today, with this technology, anybody can sequence DNA in their pocket for around US$1000. What this means is that we are rapidly moving towards a future where anybody will be able, through DNA sequencing, to learn which pathologies they are most susceptible to and implement preventative safeguards, behaviors, and precautions5. Today’s approach to prevention is based on generic suggestions for proper lifestyles. In the near future, pairing the data collected through personal genomics with the computing power of AI and machine learning algorithms, it will be possible to formulate a set of extremely personalized interventions taking into account the genetic predispositions of the individual and environmental factors, significantly delaying the onset of pathologies. But the shift to preventative healthcare enabled by personal genomics and AI will not stop at the individual level. One of the most significant trends in healthcare is that patients are increasingly willing to share their health data if in return they see a benefit to themselves and to the community6. Relying on patient consent to data sharing within the context of an international network of interoperable EHRs, collective medical data could be made available to the scientific community for large-scale processing of predictive patterns of pathologies, thus significantly supporting health research7.
Patient access to medical records
Data is regarded by many as the new gold in this digital age. When it comes to healthcare, data can make the difference between life and death as doctors rely on accurate patient medical history to make a correct diagnosis. In the past it was general practitioners (GPs) who held a complete view of the patient’s medical history. GPs, often referred to as “family physicians”, were particularly effective at this because they were often treating families across different generations, having therefore visibility over the extensive family medical history and potential genetic predispositions of the patient. While GPs remained anchored to their territory, people did not. It is now increasingly common for people to move nationally and internationally, transiting through their national public and private healthcare systems as well as through foreign healthcare systems. In this dynamic context, as data becomes more abundant and more fragmented across facilities, regions or even countries, we lack a system to collect and safely store medical data for each patient. Therefore, in the century of data, doctors often still make diagnoses relying on a medical history which only concerns the patient’s memory.
The challenge to facilitate patient access to medical records and to integrate records within an always up-to-date medical history is a complex one as it requires governments to develop a virtual space in which to effectively accumulate medical data, while ensuring the safety and interoperability of this data. Electronic Health Records (EHRs) are the obvious solution to the issue. EHRs are real-time, patient-centered digital records that make information available instantly and securely to authorized users8. EHRs contain medical and treatment histories of patients, together with information on allergies, immunization dates, radiology images and lab results. EHRs are designed to be shared among different healthcare providers. So why are we still talking about the challenges of access to medical records and medical history maintenance? Let’s take the European Union as an example. Research shows that, while over 80% of the countries in the EU have already rolled out national EHRs, often paired with appropriate legal frameworks and institutional environments, under 20% of countries in the EU have implemented fully interoperable EHRs9 Lack of interoperability means many patients may be unable to access or use their data as they switch healthcare providers, or as they transit from the public to the private healthcare system, or if they relocate. The issue with the implementation and interoperability of different national EHR systems is not only a technological one, but also a political one. Francisco Lupianez Villanueva, one of the authors of an extensive report10 on EHR interoperability from the European Commission, believes that “Europe’s healthcare systems are organized in very varied ways: they are centralized, decentralized, dependent on public insurers, private, etc. This variety means that it is difficult to create a definitive profile, which is a barrier to interoperability at the European level”11. In the case of Spain and Italy, while the level of digitization may be high, the highly decentralized healthcare system results in a lack of interoperability even within the national borders, between different regions. It is necessary to reach an agreement on a common electronic health record format in order to unlock the safe flow of health data within and across borders and ensure patients -and their doctors- will always have immediate access to their updated medical records.
[1] Dealroom
[2] Roberto Ascione, “The Future of Health”, 2022
[3] McGinnis, Foege, “Actual causes of death in the United States”, 1993, JAMA
[4]Dealroom
[5] Roberto Ascione, “The Future of Health”, 2022
[6] “Consumers expect benefits from handing over their personal data”, 08 March 2022, Hannover Re
[7] “Questions and Answers – Commission makes it easier for citizens to access health data securely across borders”, 6 February 2019, European Commision
[8] “What is an electronic health record (EHR)?”, HealthIT.gov
[9] “Interoperability of Electronic Health Records in the EU”, 13 October 2021, European Commission
[10] “Interoperability of Electronic Health Records in the EU”, 13 October 2021, European Commission
[11] Agustín López, “The electronic health record is not yet in force in the European Union”, 22 April 2022, Universitat Oberta de Catalunya



